Lymphex Research
The Mechanical–Lymphatic
Framework of Human Disease
Cranio-Caudal Drainage Bottlenecks & Tissue Stagnation
Inflammation Is the
Common Endpoint
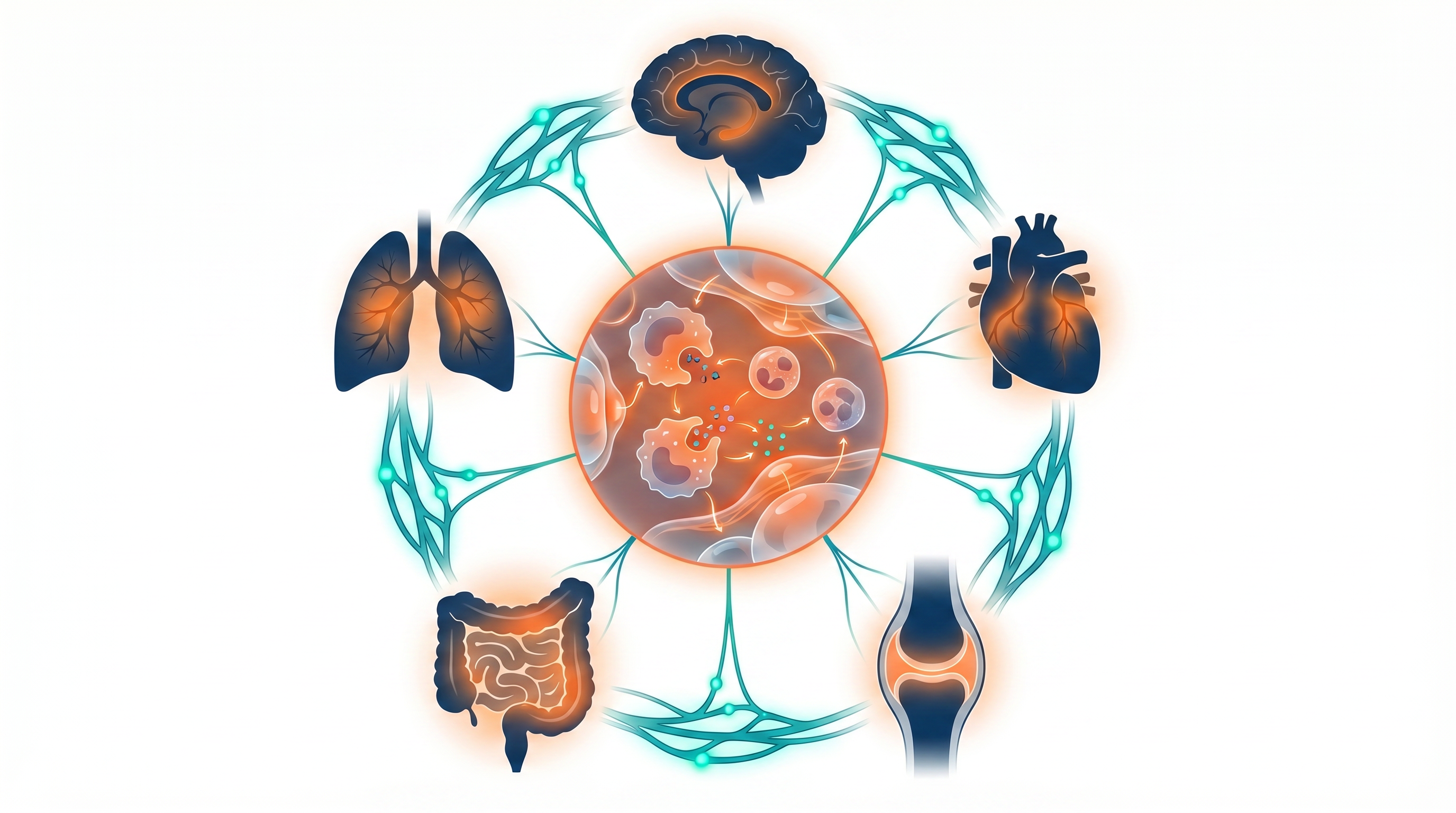
Across cardiovascular disease, neurodegeneration, autoimmune conditions, and cancer — chronic inflammation appears as a shared downstream mechanism.
Yet the upstream mechanical drivers of this inflammation remain poorly understood. What if the answer lies not in molecular pathways alone, but in the physical architecture of the body?
Drainage, Not
Circulation
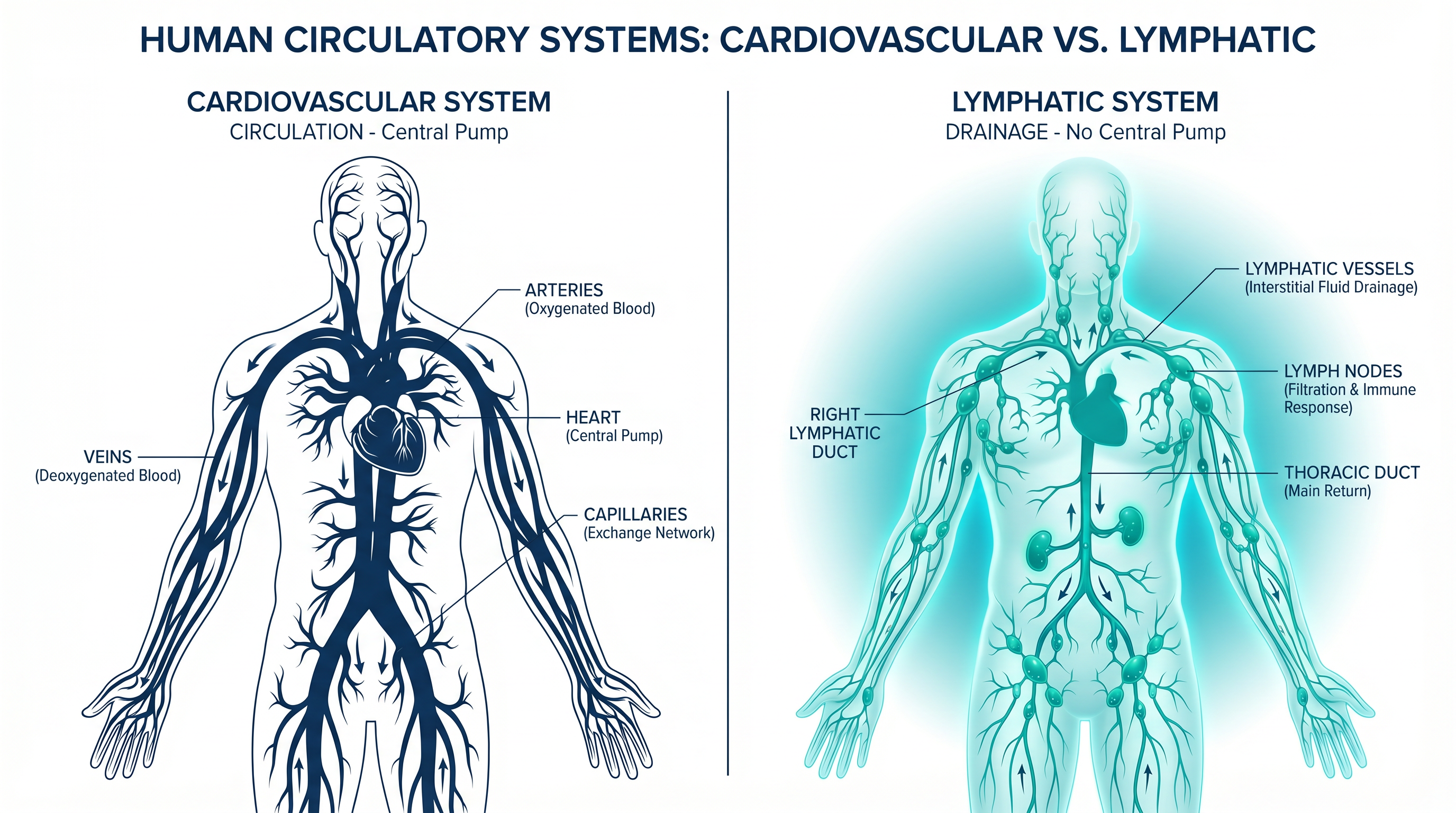
The cardiovascular system has a central pump. The lymphatic system does not. It relies entirely on movement, pressure gradients, and fascial mechanics to drain interstitial fluid.
This fundamental difference means the lymphatic system is uniquely vulnerable to mechanical disruption — and yet it remains one of the least studied systems in medicine.
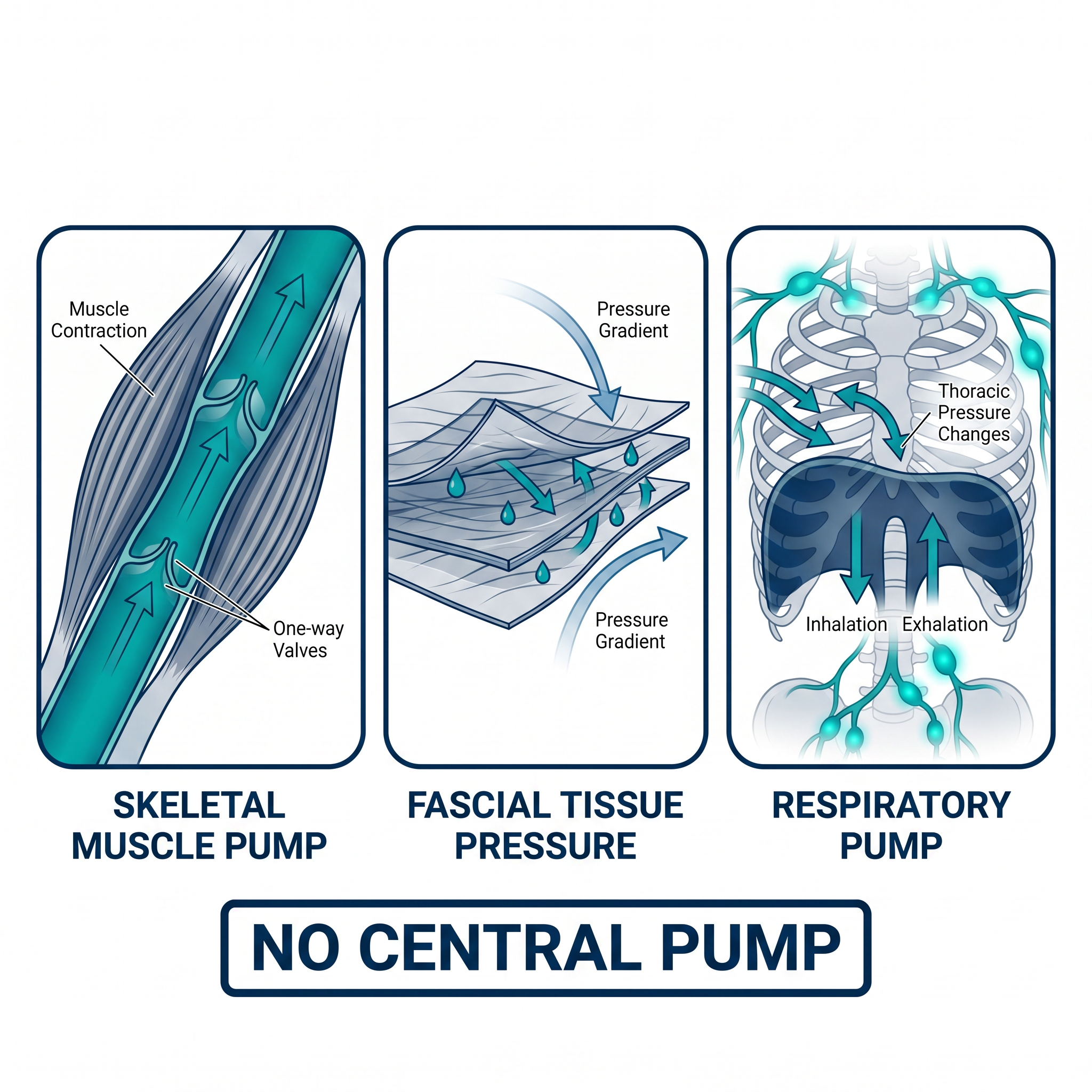
No Central Pump.
Movement Is the Pump.
Lymphatic flow depends on three mechanical forces:
Where these forces are compromised, fluid stagnates.
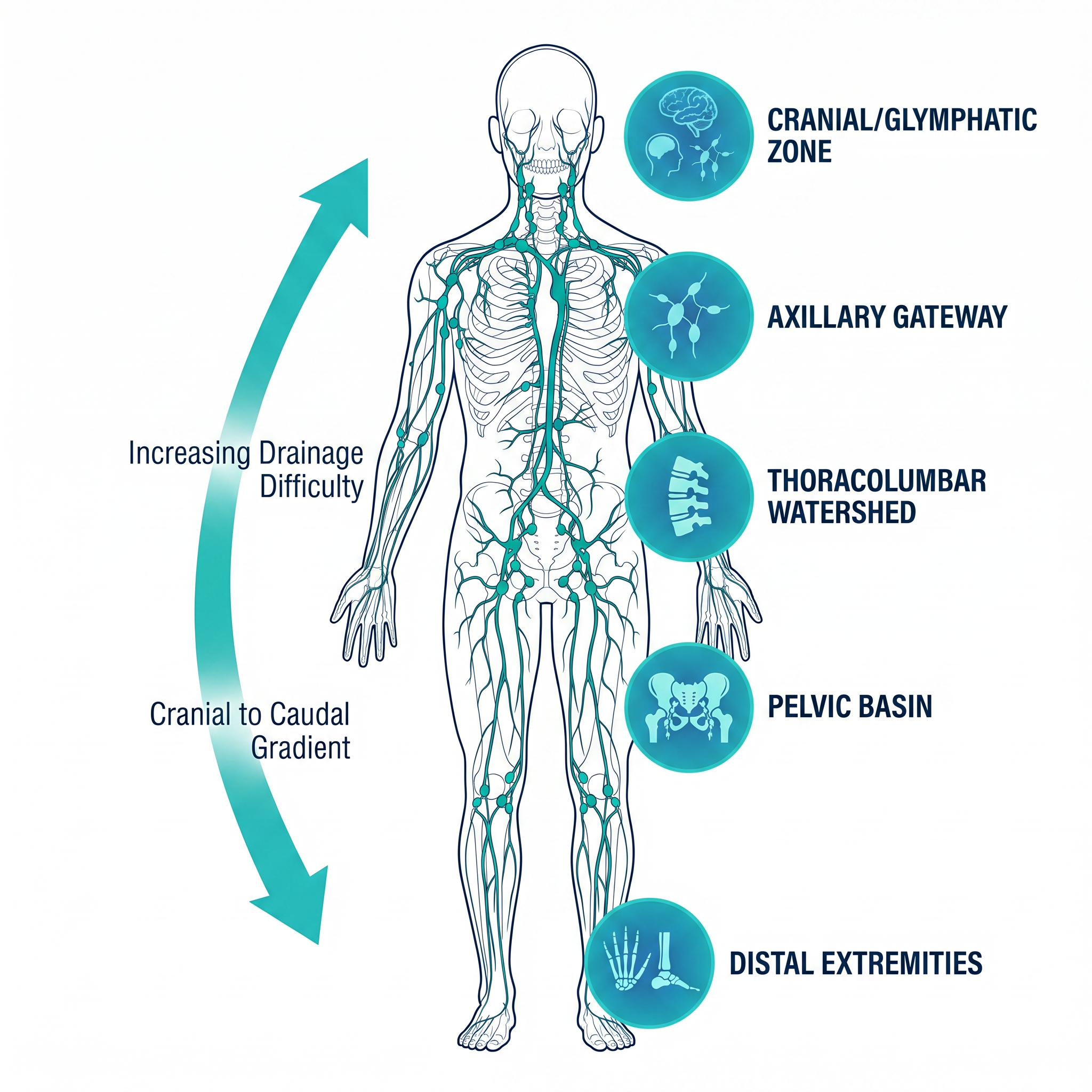
The Cranio-Caudal
Drainage Gradient
Lymphatic drainage follows a top-to-bottom gradient — from the cranium through the axillary region, along the spine, through the pelvis, and into the distal extremities.
"Where anatomy creates convergence, lymphatic stagnation can occur."
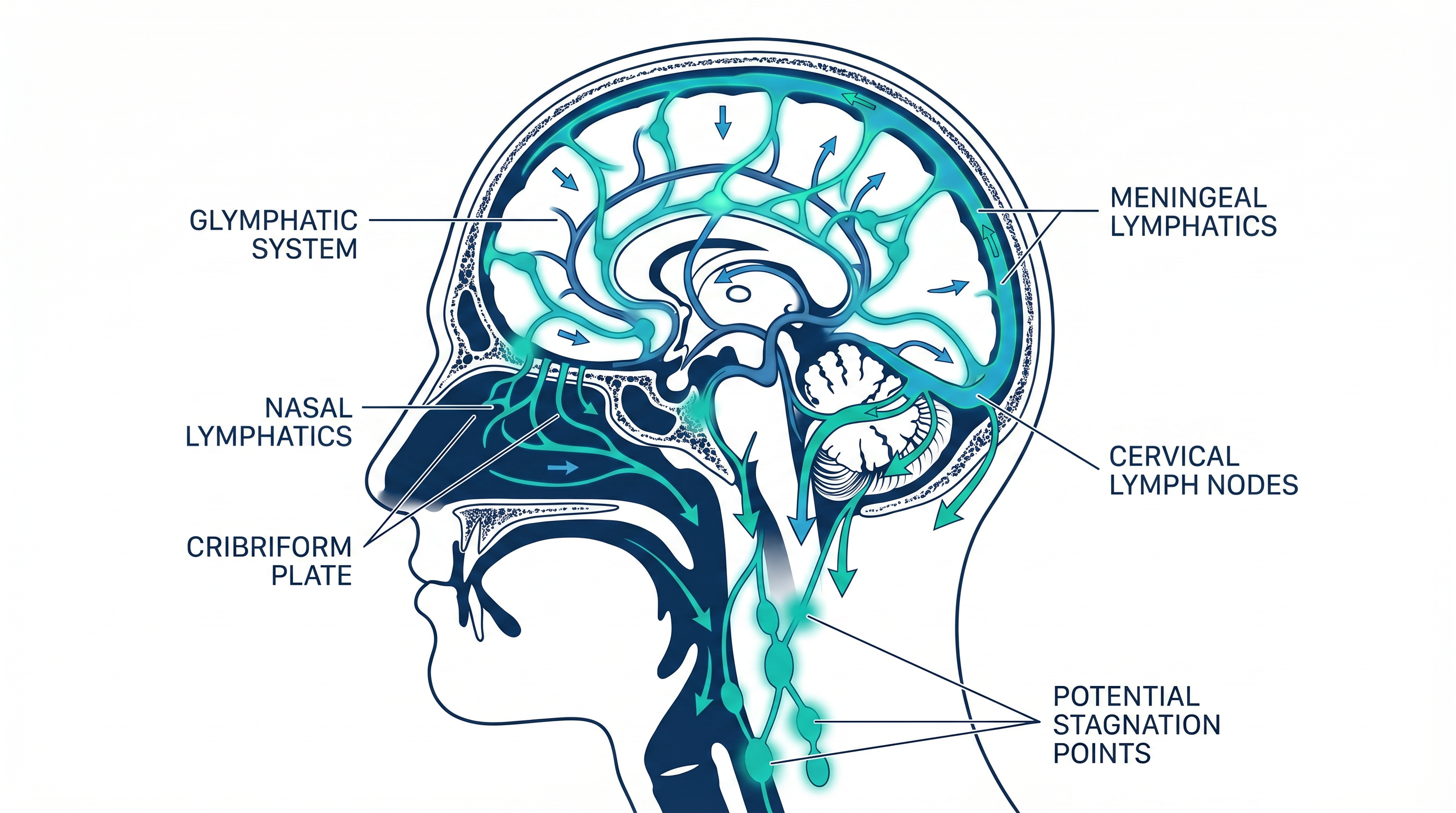
Glymphatic System &
ENT Outflow
The brain's glymphatic system clears metabolic waste during sleep through perivascular channels. This flow converges with meningeal lymphatics, sinuses, and deep cervical pathways.
Disruption at this level may contribute to neuroinflammation and neurodegenerative conditions.
The Axillary Gateway
Both armpits serve as the primary lymphatic convergence zone — where upper limb, thoracic, and breast drainage pathways meet. Modern lifestyle patterns (sedentary posture, restricted shoulder mobility) may create chronic compression at this critical junction.
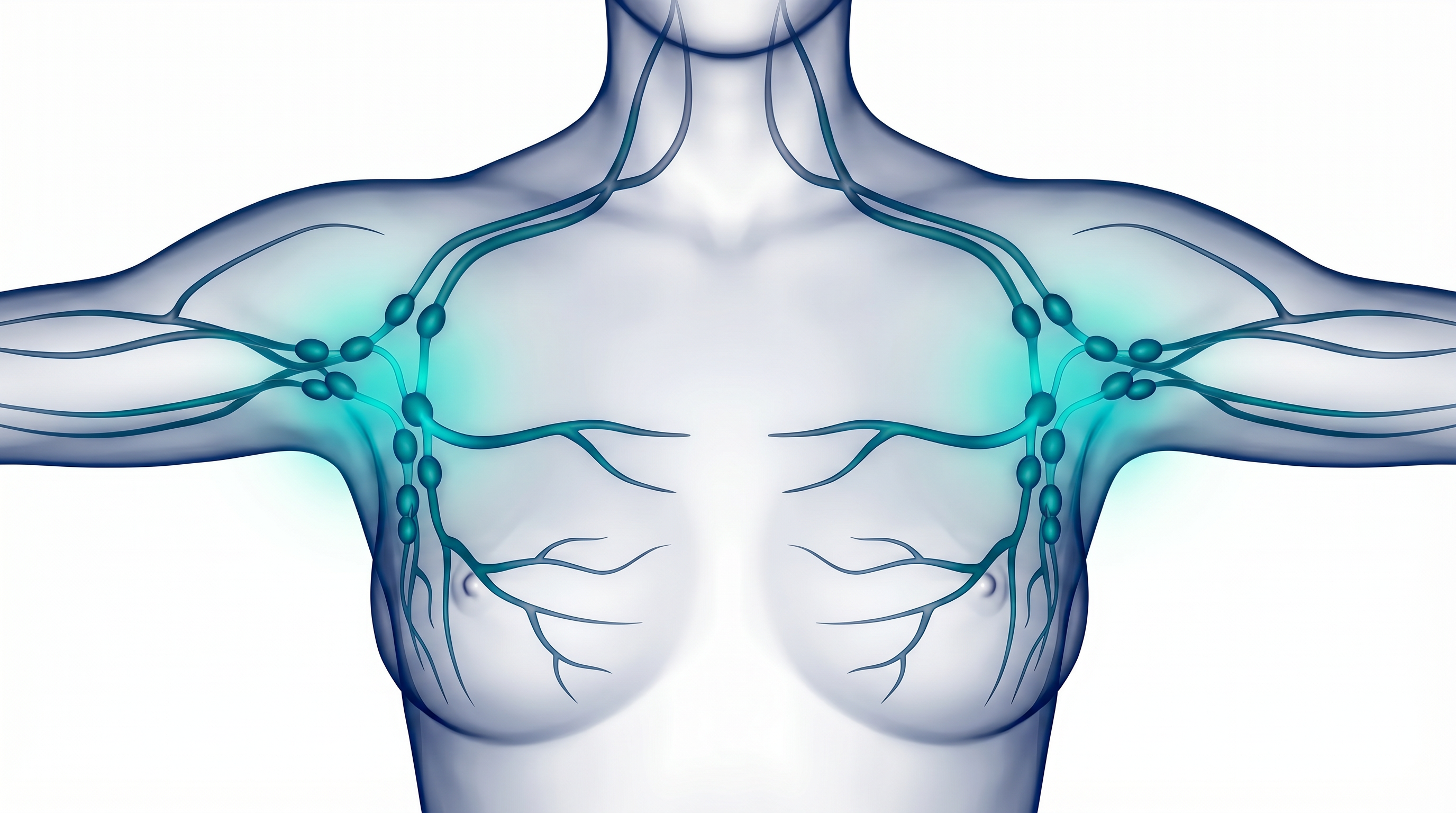
Primary lymphatic convergence zone
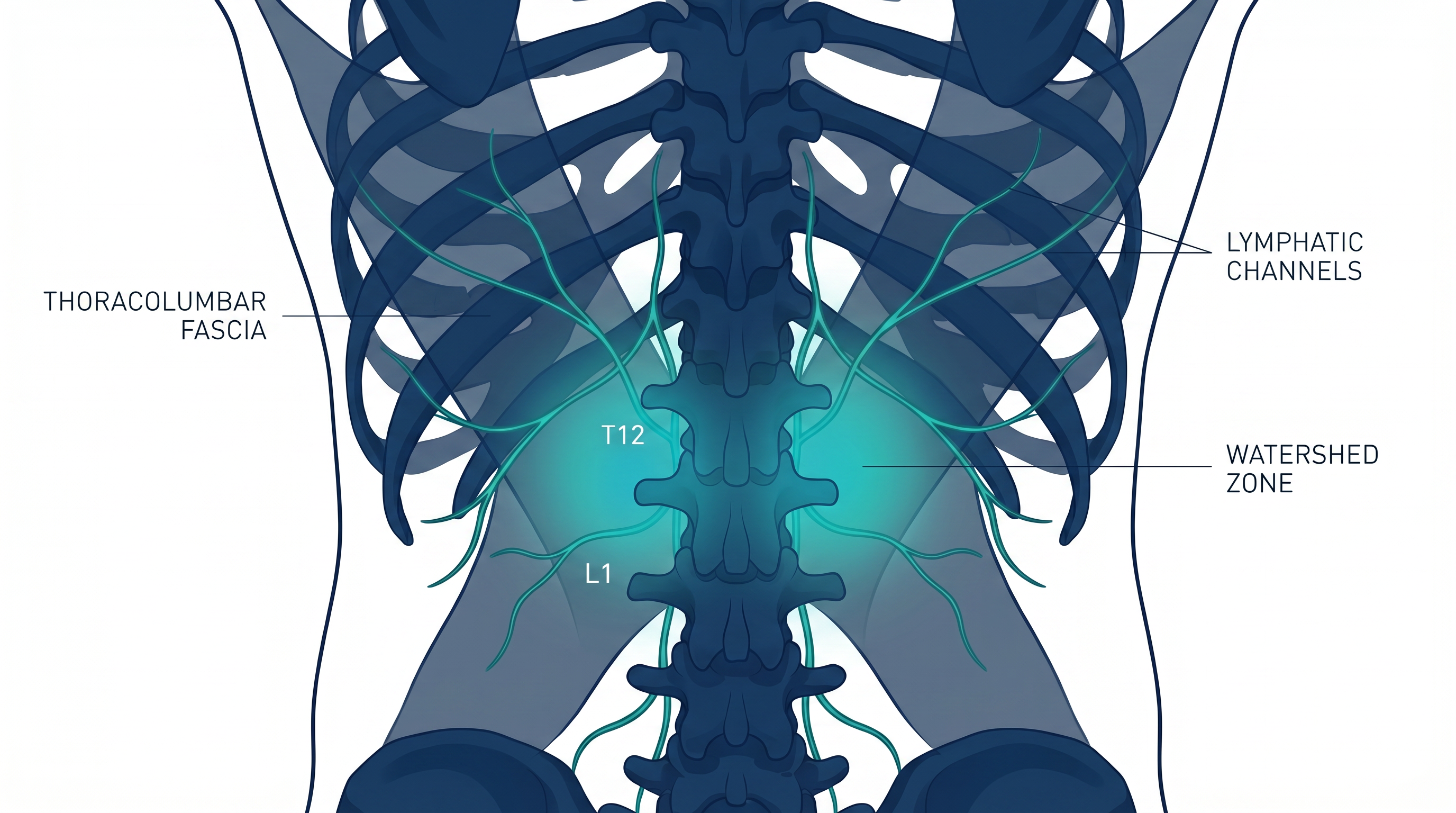
Spinal & Fascial
Transition Zone
The thoracolumbar junction represents a critical watershed where spinal mechanics and fascial tension patterns converge. Changes in spinal curvature and fascial stiffness at this level can disrupt lymphatic flow between the upper and lower body.
This region is particularly sensitive to postural dysfunction and may represent a key bottleneck in the cranio-caudal drainage pathway.
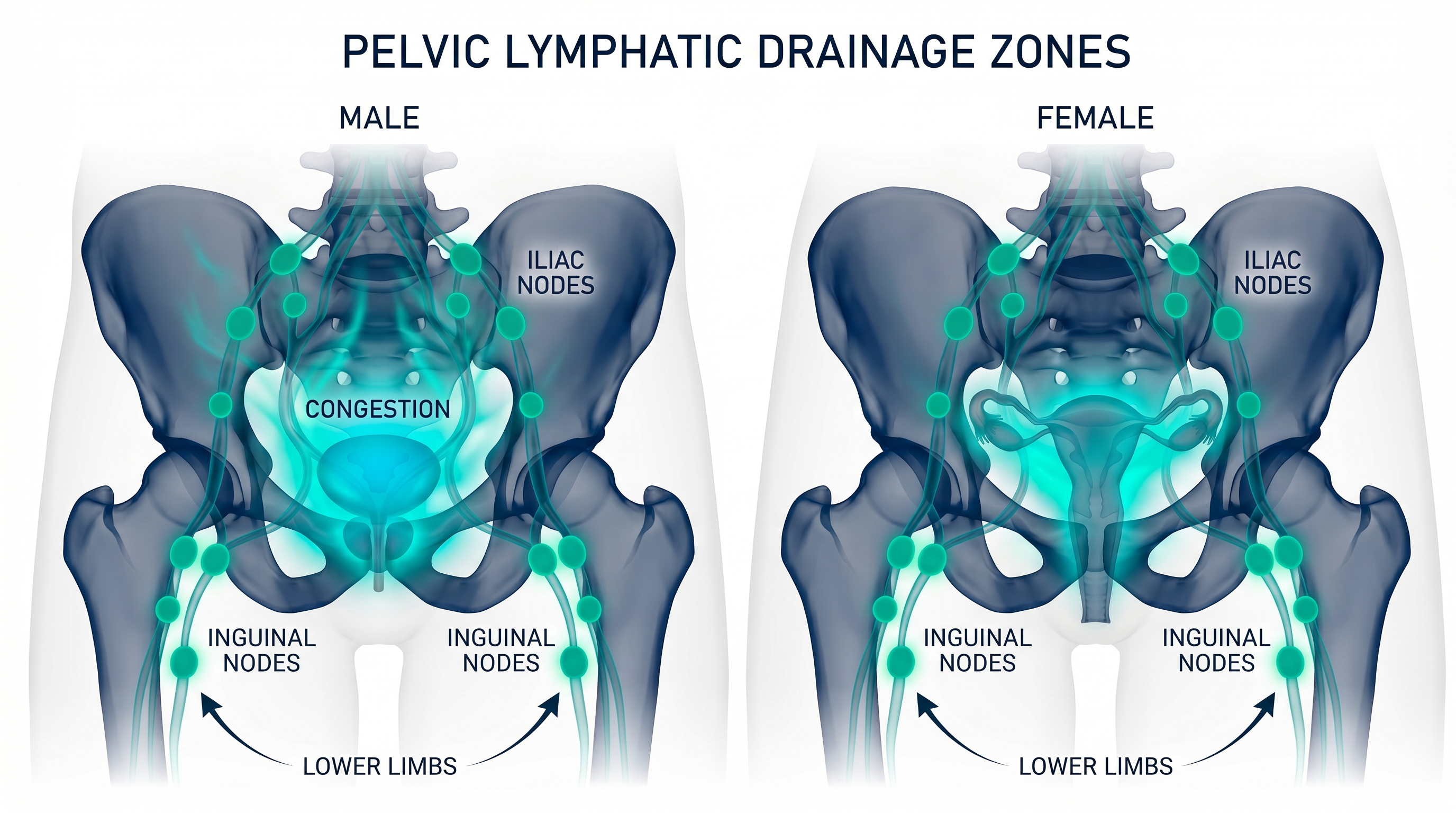
Pelvic Congestion
Patterns
The pelvic basin is a natural collection point for lymphatic fluid from the lower body. Both male and female anatomy create unique congestion patterns where fluid can accumulate.
Prolonged sitting, reduced hip mobility, and fascial restrictions may exacerbate stagnation in this region, potentially contributing to pelvic inflammatory conditions.
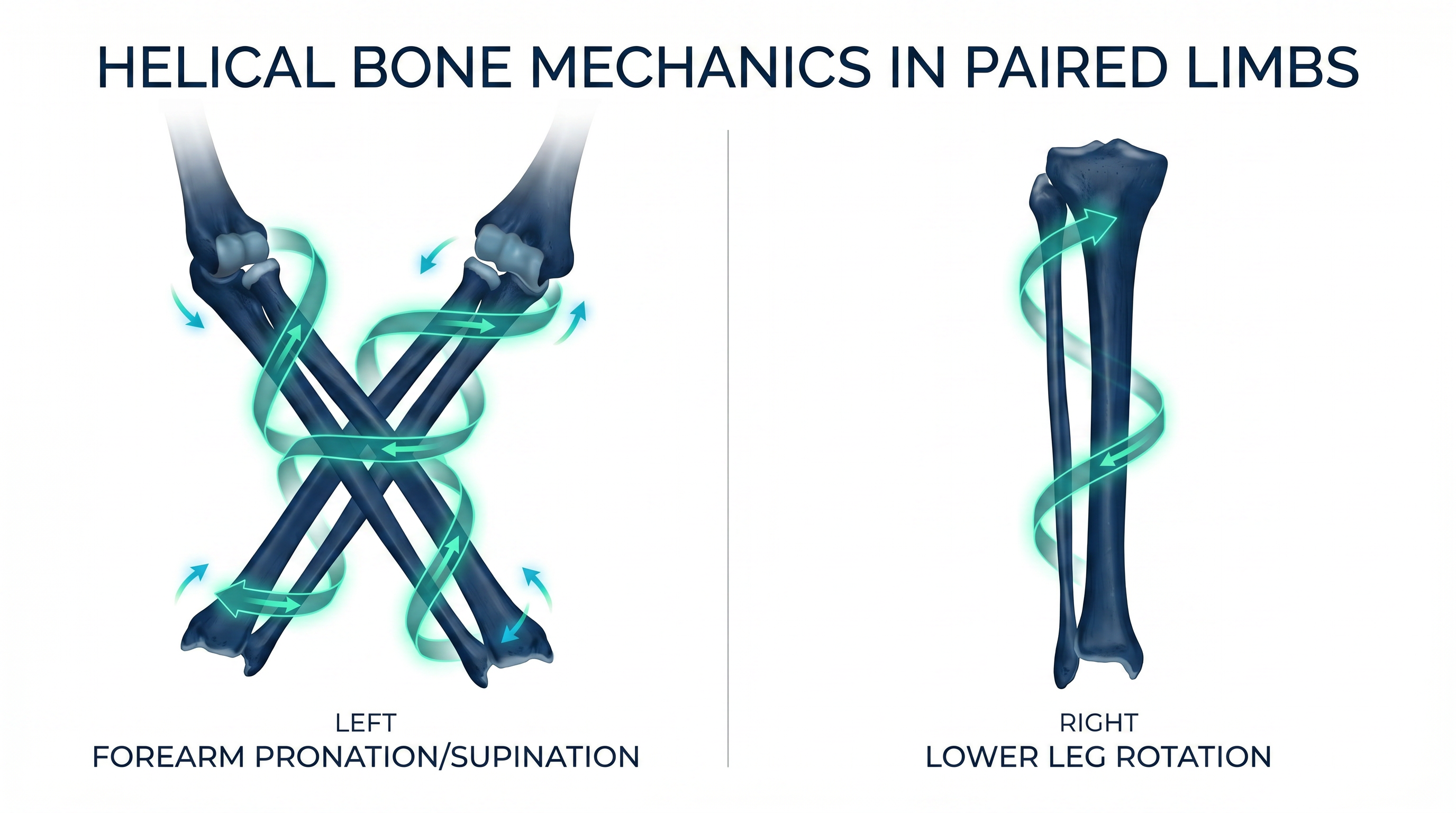
Spiral Mechanics of
Paired Bones
The radius/ulna in the forearm and tibia/fibula in the lower leg create helical rotation patterns during movement. This spiral mechanic may function as a natural pump for lymphatic and interstitial fluid transport.
When rotational range of motion is restricted, this pumping mechanism is compromised — potentially contributing to distal fluid stagnation.
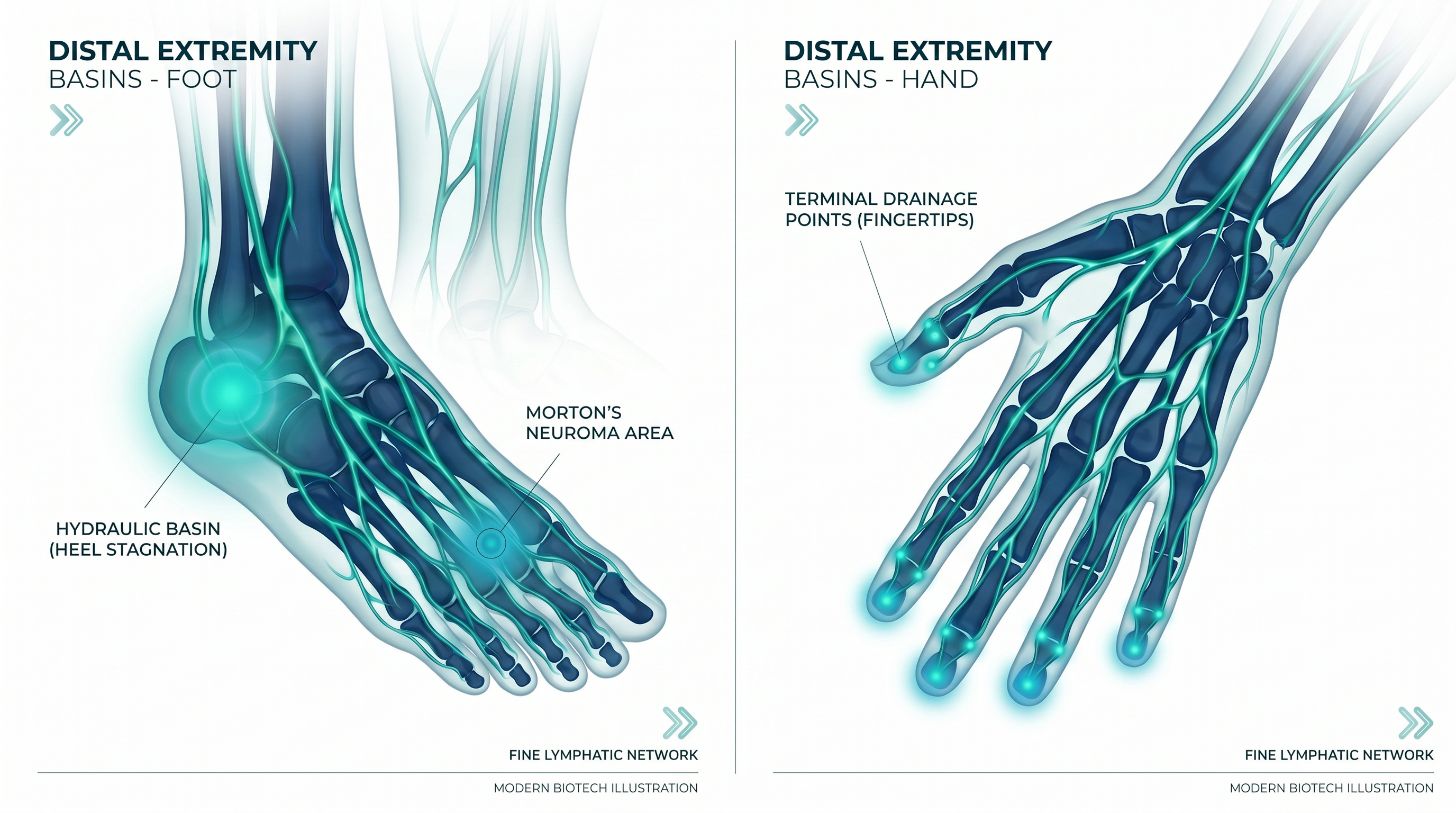
Terminal Drainage
Zones
The hands and feet represent the terminal points of lymphatic drainage. Fine lymphatic networks in these regions are particularly vulnerable to stagnation due to their distance from central drainage pathways.
Hypothesis example: Morton's neuroma may represent localized lymphatic stagnation and inflammation in the intermetatarsal space — a terminal drainage zone with limited mechanical clearance.
Where Anatomy Creates Bottlenecks
Upper Arm
Humerus → radius/ulna transition
Wrist
Radiocarpal joint compression
Hand
Opposing thumb, thenar/hypothenar
Cuticles
Terminal drainage endpoints
Leg
Tibia/fibula rotational restriction
Ankle
Convergence joint
Heel
Hydraulic basin
Toes
Terminal drainage endpoints
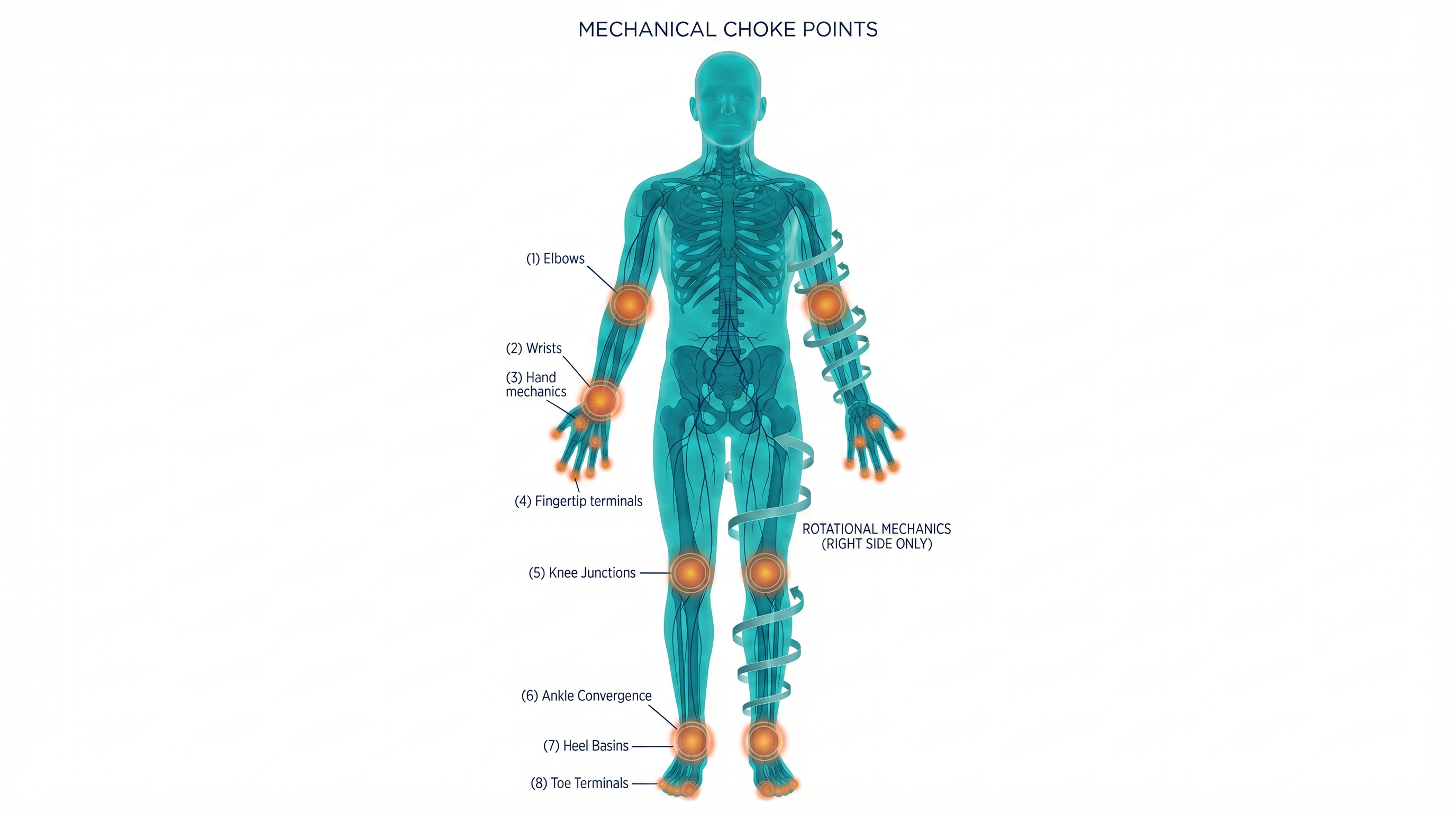
The Mechanical–Lymphatic Framework
A comprehensive view of cranio-caudal drainage bottlenecks and tissue stagnation points
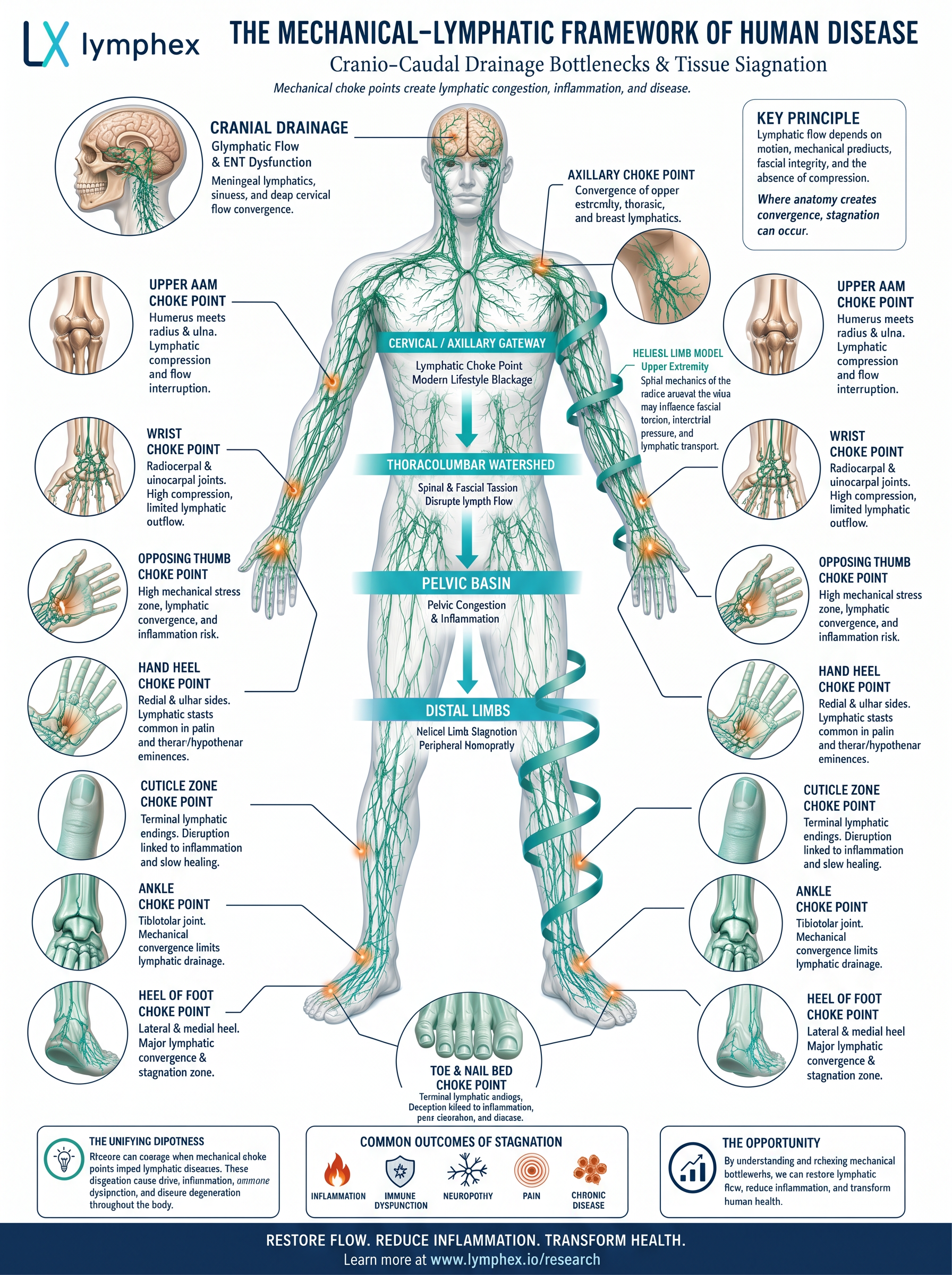
The Integrated Pathway
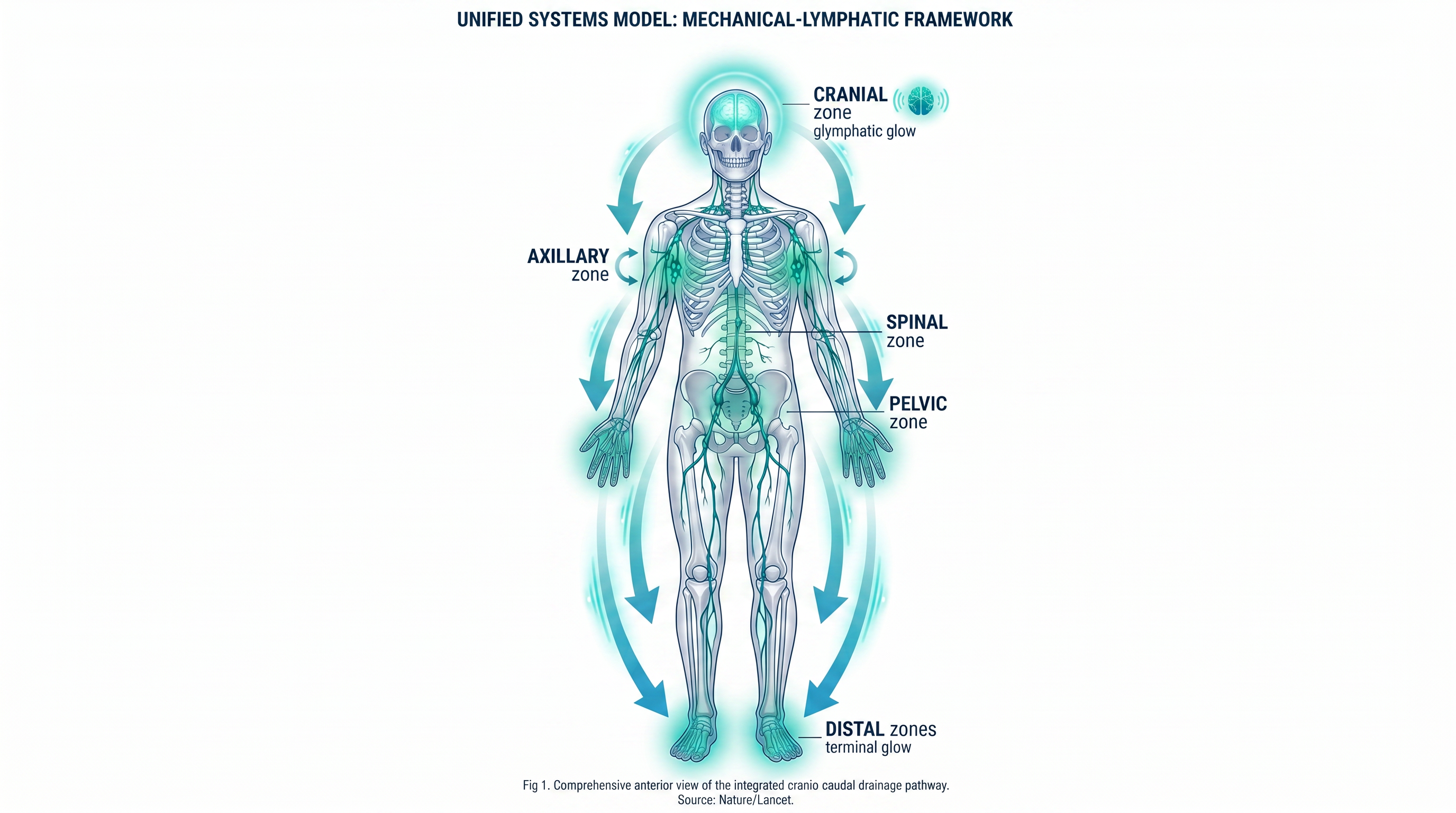
Cranial
Glymphatic clearance
Axillary
Primary convergence
Spinal
Fascial watershed
Pelvic
Collection basin
Distal
Terminal drainage
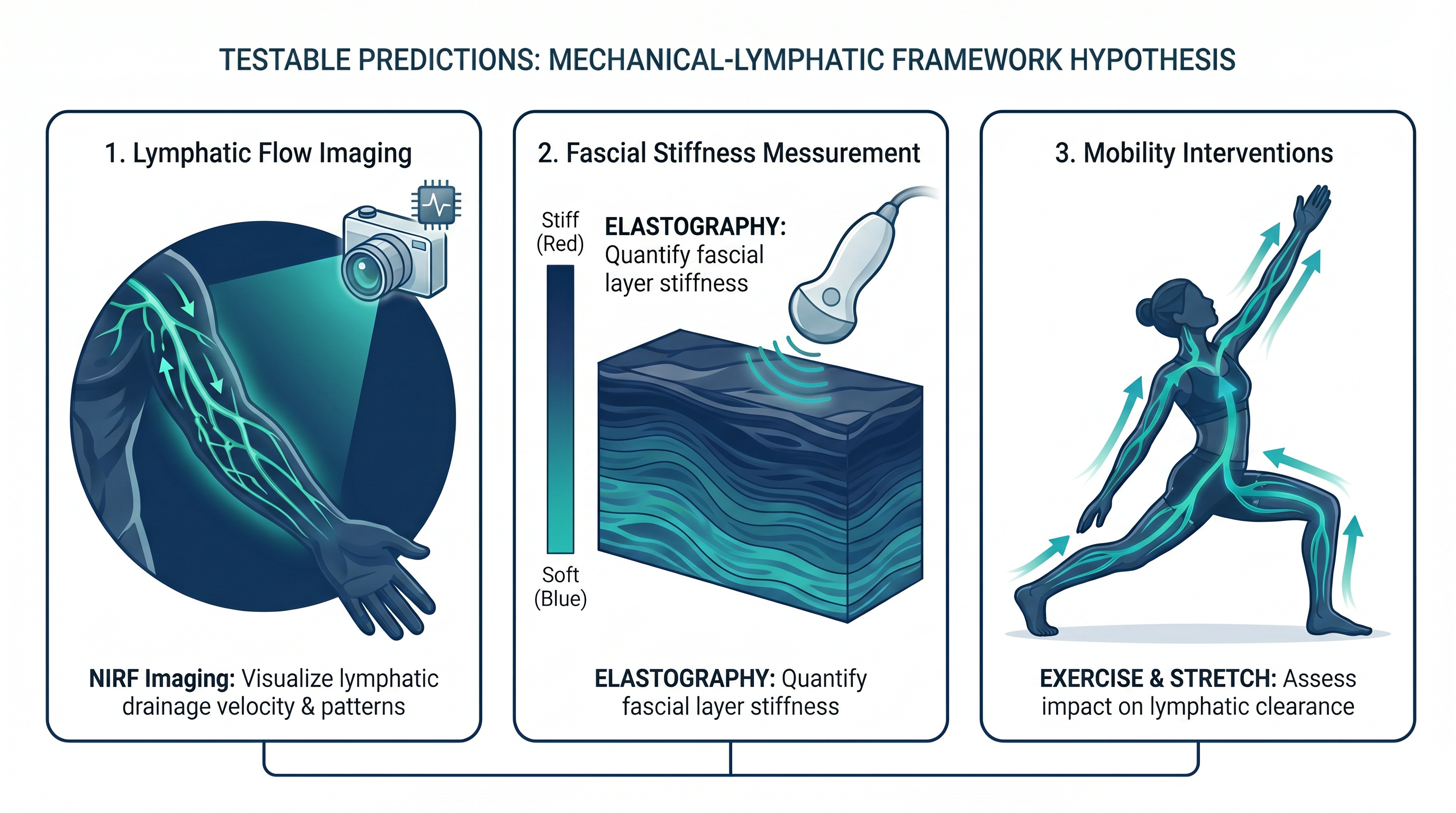
A Falsifiable
Framework
Lymphatic Flow Imaging
NIRF imaging to visualize drainage velocity and identify stagnation zones in vivo
Fascial Stiffness Measurement
Elastography to quantify fascial layer stiffness at predicted choke points
Mobility Interventions
Assess whether targeted movement protocols improve lymphatic clearance at bottleneck regions
A Simple, Coherent Model
Worth Investigating
"Mechanical anatomy and lymphatic transport may represent an overlooked dimension of human physiology."
This framework connects mechanics, lymphatic flow, interstitial fluid dynamics, inflammation, and disease into a testable hypothesis. We believe it deserves rigorous scientific investigation.
